Personalised dosimetry of CT perfusion imaging
Radiation dose is the limiting factor for clinical application of dynamic CT. The accurate measurement of tissue perfusion requires the sampling of contrast agent uptake during a dynamic scan. Therefore low dose protocols have been proposed by vendors and in the literature. The physical standard developed in WP1 will allow the study of different protocols with respect to the accuracy in the determination of the perfusion parameters. However, the dose depends not on the system parameters alone but also on the size and shape of the patient.
The aim of this work package is to lower the high uncertainties of the effective dose estimates for one organ from 20 % 50 % to significantly lower levels of 10 % 20 % and to establish and verify a general procedure for Patient-Specific-Dose-Estimates (PSDE) in computed tomography (CT) imaging with special application to CT perfusion studies. The procedure is based on the calculation of the post-scan 3D dose distributions within the exposed parts of the patient’s body using the commercially available software package ‘ImpactMC’. This package enables the users to perform a fast Monte Carlo simulation of the complete scan. Inputs needed for such a simulation are the reconstructed CT-image (DICOM file) of the patient and anthropomorphic model extensions for scatter contribution, the scanner source model and the actual scan protocol parameters.
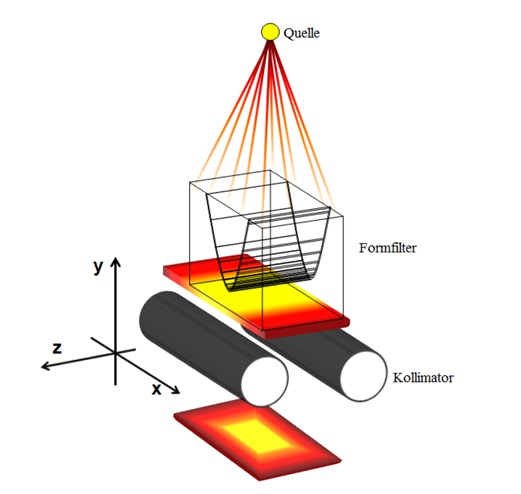
Three tasks are identified for this work package. An essential part of the scanner needed for the simulation are the x-ray beam properties, i.e. the tube characteristics described by the emitted photon fluence spectrum, the fixed filtration and the beam shaping filter, usually called ‘bow tie’ (BT) filter. Photon fluence spectra and the material and shape of the BT-filter are usually not known or proprietary information. However, non-invasive experimental methods are available to determine at least a good approximation to the x-ray spectra and material equivalent representations of the BT-filters. These data usually designated as ‘equivalent source models’ can then be used as inputs to the MC simulation program.
The first task in WP3 is to develop, construct and verify a mobile apparatus and the corresponding evaluation software for the non-invasive determination of equivalent source models that are well suited for on-site measurements at CT machines in a clinical environment. The second task is to verify calculated 3D dose distributions by measurements with dosimeters in anthropomorphic phantoms at different scanner types. The third task is to apply the new dose estimation procedure to studies in CT perfusion imaging including those conducted with the newly developed physical standards of WP1. The objective is to provide a dose estimate in connection with the use of the physical standard of WP1 and provide estimates of the minimum dose needed to obtain a feasible evaluation data set according to the methods derived in WP2.
Mobile equipment for determination of equivalent CT source models